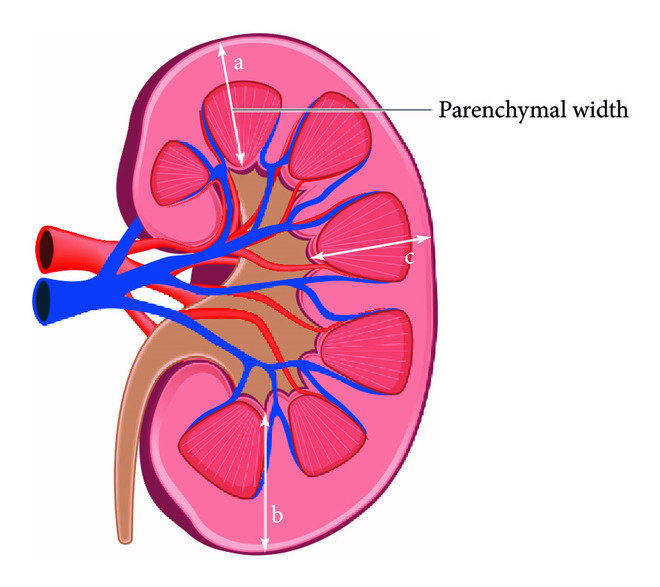
Dive into this comprehensive guide to explore kidney anatomy, physiology, and how to keep these incredible organs healthy. The kidneys are vital organs that perform life-sustaining functions, such as filtering blood, maintaining fluid balance, and excreting waste. 1) Normal Anatony: Abdominal quadrant and it’s content abdominal organs by region adults kidney are like bee shape structure organ that are retroperitoneal is location they are normally located high in abdominal cavity and against its back wall lying on either side of the 12th Thoracic and third lumbar vertebral and outside the peritoneum the membrane that lines the abdomen and abdominal organs. The kidney in the vetropertoneal cavity near the posterior body wall just below the diaphragm the lower ribs protect both kidneys the left kidney is located higher than the right kidney because of the size of the liver which occupy most of the right upper side quadrant of the abdomen. The urinary system consists of the right upper urinary tract kidney and ureter and the lower urinary tract bladder and urethra the functional unit of the kidney is the nephrons Relationship of the kidney supernal gland adrenaline and vascular structure to on another. 2) Physiology: The kidneys are vital organs responsible for maintaining homeostasis. They perform several crucial functions: Kidney Anatomy: Anatomically, the kidney is enclosed by three layers: The renal medulla, the innermost part of the kidney, is responsible for urine concentration. Renal Parenchyma: Each kidney is composed of two main regions: The renal pyramids, composed of renal medulla, are separated by renal columns, extensions of the cortex. The renal pelvis, a funnel-shaped structure, collects urine from the renal calyces. Urine flows from the renal papillae through the minor calyces, major calyces, and renal pelvis into the ureter. Normal cortical thickness in adults ranges from 0.8 to 2.5 cm. Location: The kidneys are retroperitoneal organs located in the lumbar region of the abdomen. They extend vertically from the 12th thoracic vertebra to the 3rd lumbar vertebra. The right kidney typically sits slightly lower than the left due to the position of the liver. Both kidneys are positioned posterior to the parietal peritoneum and anterior to the posterior abdominal wall muscles. Shape size weight and orientation: Each kidney is about 11cm broad and 3cm thick the left kidney is a little bit longer and narrower then the right kidney on an average the kidney weight is 150g in males and 135g in females the kidney are reddish brown in color. Ureter: The ureter are a pair of narrow ones thick wall muscular tubes which convey urine from the kidney to the urinary bladder they lied dead to peritoneum closely applied to the posterior abdominal wall in the upper part. There are two locations of each kidney the size is 10 – 12 inches 30 – 25 cm long and the diameter ¼ inches 6_8 mm the location is behind the abdominal cavity Anatomy and Physiology Function: The ureter function is a transparent lots of time urine from the bladder to the kidney persistent urine back flow the kidney. The main part of ureter are is a Renal pelvis the collection of urine and proximal URETER behind the kidney. Condition Of Ureteral: Issues: The main issues of ureter disturbance is: The treatment options is surgery endoscopy and mediation.. the doctor for patients is intake lots of water because of reasons healthy lifestyle or healthy kidney Physiology function: Excretory function: Regulatory functions: Synthetic function: Kidney synesthesia new substances like: Endocrine function: JG cell secrets Rennie in response to decrease renal arterial pressure and increase renal nerve discharge B1 effect Sonological Pathology of Kidney: Nephritis: The inflammation of kidney is called nephrolithiasis Cause: Clinical features: Sever pain and tenderness in the lumber region Sonological finding: In ultrasound we find inflammation in grade I parenchyma changes and grade II & grade III parenchyma changed Masses In Kidney: We maybe findthe following types of masses in kidney Solid Masses: Often we find solid mass in the kidney but this mass might be possible single or multiple and if different size. The outer margin of the mass are mostly which is suggestive for benign tumor or nephroma but sometimes irregular masses seen which is suggestive for malignant tumor or Nephron carcinoma Kidney Stones: The pressure of stones in kidney is very common called nephrolithiasis it’s mostly in seen in cortical region the stones maybe single or multiple or in different sizes. The stone may be present in upper middle lower portion of the kidney in majority of the patients Clinical Features:
Top 5 Causes of Urinary Tract Infections: Symptoms, and Treatments
Learn about the causes, symptoms, diagnosis & treatment of urinary tract infections, including uncomplicated and complicated UTIs, recurrent infections & more. Urinary Tract Infections: presence of microorganisms in the Urinary Tract Infections that cannot be accounted for by contamination. The organisms have the potential to invade the tissues of the urinary tract and adjacent structures. Definitions: Microbiology: Clinical Presentation: Diagnostic Studies: Treatment: Treatment And Symptoms Of UTI? It can involve any part of your urinary system. Bacteria especially E. coli are the most common cause of UTIs. Symptoms include needing to pee often, pain while peeing and pain in your side or lower back. Antibiotics can treat most UTIs. Main Cause Of Urinary Tract Infection? UTI s typically occur when bacteria enter the urinary tract through the urethra and begin to spread in the bladder. The urinary system is designed to keep out bacteria. But the defenses sometimes fail. When that happens, bacteria may take hold and grow into a full-blown infection in the urinary tract. 5 Warning Signs Of Bladder Infection? Symptoms of lower UTI Include: Can I Treat Urine Infection Myself? If you have a mild UTI, it might go away on its own over a few days. If you’re not pregnant or at higher risk of developing a complication from a UTI, you may be able to hold off on antibiotics for a couple of days to see what happens. Get medical care if your symptoms don’t start to improve after a couple of days. What Is The Fastest Way To Treat UTI? It’s standard for a doctor to prescribe antibiotics for UTI treatment. After starting antibiotics therapy, symptoms usually improve within 2–4 days . Many doctors prescribe an antibiotic for at least 3 days. If the UTIs don’t clear up after antibiotic therapy, it may mean that you need a different type of antibiotic.
What Are The Symptoms And Causes Of Ascites?
In this blog , we are going to discuss about causes, symptoms and treatments What Is Ascites? Ascites can be defined as a medical condition that entails the accumulation of excessive fluid in the peritoneal cavity, which is located between the abdomen lining and adjacent abdominal organs. Therefore, it produces major protuberance in the stomach hence some people call it different names such as peritonitis, hydroperitoneum, and so forth. It is not a standalone disease but rather a manifestation of many underlying health problems in humans which may be severe. Causes, Symptoms, and Treatments: Gross Appearance of Ascites Fluid: The ailments and understanding that ascites diagnosis as well as understanding ascites diagnosis from a clinical standpoint rely on the gross appearance of the fluid. This fluid can inform us significant information about the underlying problem that has led to its accumulation. Color of Fluid: 1) Translucent Or Yellow: This is often a sterile or normal fluid. The occurrence of a translucent or yellowish shade indicates that the fluid might have low infectivity and/or contamination. This can be observed in cases where the ascites are not associated with an infection but due to cirrhosis of the liver. 2) Brown: A brownish coloration is connected with hyperbilirubinemia. Hyperbilirubinemia describes a situation where there is more than enough bilirubin in blood which in turn can be linked to conditions of the liver and also blockage of bile ducts. 3) Bilirubin: Bilirubin, which results from normal breakdown of red blood cells, could get deposited in the liquid found within the cavity in case it accumulates owing to liver’s incapacity for the treatment process. 4) Cloudy Or Turbid: Evidence of infection is usually shown by turbid or cloudy fluid. The white blood cells, bacteria or other inflammatory cells are the reasons for the frequently cloudy fluid. In other words, the body has an inflammatory reaction against a pathogen which could be one of the following: bacteria, viruses or fungi. On paracentesis, the ascitic fluid appeared milky and turbid. 5) Pink Or Blood-Tinged: There may be pinkish or blood-tinged fluids in mildly traumatized cases. It occurs when there is slight bleeding into the abdomen which is likely to be from a recent injury or through any surgical procedure done that damaged blood vessels present. 6) Grossly Bloody: If there is grossly bloody fluid this indicates malignancy chances exist. Blood-stained ascitic fluid indicates the spread of cancer particularly abdominal and gastric cancers to the peritoneum lining or other abdominal organs. Causes of Ascites: The development of ascites can be attributed to several underlying causes, each of which includes complex physiological processes. To do accurate diagnostics and prescribe treatment, it is crucial to comprehend these factors. Liver disease is the most common cause of ascites Ovarian Cancer and Ascites: A Hidden Connection Signs And Symptoms of Ascites: Although the development of ascites shows remarkable differences which can be attributed to the amount of fluid and etiology involved, there is little change in external appearance at first. Sometimes in the early days, there may be no symptoms without a rate of development that is high enough to trigger them. Common Signs And Symptoms Include: Gastroesophageal reflux disease (GERD), also known as acid reflux or heartburn, is a chronic digestive disease. Grading System For Ascites: Ascites are commonly categorized based on their severity, allowing for informed results on treatment and displaying how fast or slow the disease progresses. The grading system for ascites can be divided into three groups: Grade 1: Mild Ascites: Grade 2: Moderate Ascites: Grade 3: Large Ascites: Prevention And Control Of Ascites: Ascites, often a result of liver disease, heart failure, or other medical issues lead to the build-up of fluid in the abdomen. A combination of lifestyle changes and medical interventions are needed for managing and preventing it. Below are key strategies for the prevention and control of ascites: Sonographic Features Of Ascites: The peritoneal cavity, normally empty of liquid, is the space lying between the abdominal lining and the abdominal organs in a healthy person. During an echo graphic examination, the absence of expression in this cavity is a normal finding. The earliest detectable fluid accumulation due to effusion is usually found in abdominal recesses like the hepatorenal angle or Morrison’s pouch which is located between the liver and the right kidney. Even as little as ten milliliters of fluid can be characterized from this area using high-resolution ultrasound. The image above organizes an example of how ascites will appear on abdominal ultrasound Nevertheless, peritoneal effusions are not all neat or devoid of other fluids. Blood, pus, or other particulate matter may sometimes blend in with the effusion. This condition may give rise to internal echoes which are seen on ultrasound images. Such internal echoes appear as spots or more solid areas scattered throughout echogenic liquid. Investigating these internal echoes can reveal very valuable information concerning ascites’ origin. For example, seeing them indicates hemorrhagic ascites (containing blood), infected ascites (containing pus including inflammatory debris) or chylous ascites (containing lymphatic fluid with fat). Therefore, it can be said that ultrasonographic characteristics of ascites comprise the detection of any fluid in the places where there is no hepatorenal angle and its ultrasound presentation without any echo. Internal echoes found within the fluid may indicate that this form of ascites has been complicated by blood, pus, or other components. Treatment of Ascites: The management and treatment of ascites depend on the underlying cause and also how serious it is. Paracentesis, which mainly involves fluid removal from the peritoneal cavity, is one of the main treatments for ascites. Before paracentesis can be approved, fasting may be necessary. This helps to reduce the risk of complications during the procedure such as nausea or vomiting, which can happen if someone has an empty stomach. In paracentesis, the patient is positioned in a way that allows fluid to pool in one area of the abdomen for easy access. Generally, ultrasound guidance is used in conducting paracentesis so that doctors can pinpoint the precise location of the fluid and avoid damaging nearby
Myocardial Infarction Symptoms | Latest Treatment And Challenges
In this blog we are going to share the basic challenges and treatment of myocardial infarction symptoms. Coronary atherosclerotic cardiovascular disease and acute myocardial infarction (MI) are still some of the major contributors to high rates of morbidity, mortality, disability, and limited treatment options available. For this reason, these two circumstances have always been important to cardiologists, leading to significant research and improved treatment outcomes. Although pharmaceutical and therapeutic approaches for myocardial ischemia-reperfusion are continually improving, the annual incidence rate of heart failure is rising. Researchers believe therapies that do not directly target the infarcted myocardium cause this situation. Some examples include medications, rehabilitation, or reperfusion therapy after an ischemic injury. These approaches offer help but do not fully address the problem. Therefore, there is a persistent and growing case of heart failure following myocardial infarction, as there is no intervention targeting root causes such as myocardial disturbance or damaging mechanisms that cause a decline in cardiac function over time. This involves examining the stages of therapy but also highlights the need for new methodologies in treating patients with this disease. Nanoparticles may present themselves as viable prospects because they possess together remedial and preventive properties for acute myocardial infarction (MI). These new multidimensional nanoparticles may be more effective against the disease. Although many advances have led to decreased mortality from acute myocardial infarction, there is still a lot to be done in reducing heart failure rates. As a result, current studies on these Nano-sized particles mark a move towards better management of myocardial dysfunctions accompanied by their associated complications. Introduction: Cardiovascular disease is the number one cause of death globally, with approximately 31% of all global deaths falling into this category. Out of these, myocardial infarction (MI) is particularly deadly and it causes 13% of heart-related deaths. The closure of the coronary artery causes MI (myocardial infarction), hence preventing blood from flowing to the heart either partially or completely. This pause in the flow of blood leads to the death of the surrounding myocardium. Since the heart has a limited capacity to regenerate cardiomyocytes endogenously, eventually fibrous cells replace the lost myocardium cells. This process of replacement leads to the poor contractile ability of the heart, often resulting in end-stage heart failure. Standard treatments for MI include thrombolytic therapy, immediate percutaneous coronary intervention (PCI), and administration of lipid-lowering medications and anticoagulants. These approaches have proven effective in reducing infarction size and mortality rates. For example, percutaneous coronary intervention can restore blood flow through the affected coronary artery. However, this procedure carries the risk of ischemia-reperfusion injury, leading to additional tissue damage and myocardial cell apoptosis. In the end, these complications may contribute to heart failure and other negative health outcomes. Post-MI pathological changes within the body, such as the production of reactive oxygen species, mitochondrial dysfunction, and calcium overload, worsen the problems. These changes cause cell death and inflammatory responses that hinder the recovery process. Despite the existence of anti-inflammatory and antioxidant medication, their efficacy is usually reduced by limited specificity, low bioavailability, and short half-life. Hence, there is an urgent need for safer and more economical ways to prevent and manage myocardial infarction. Current Practices: Extensive research and discussions over the past decade have informed current therapeutic practices on myocardial infarction. For instance, healthcare providers should administer thrombolytic medications at the earliest possible time for maximal benefit. However, thrombolysis may only be fully effective if administered up to 12 hours after symptoms appear. Healthcare providers can use audit reviews to help ensure timely administration by monitoring and improving the timing of thrombolysis. Additionally, healthcare providers must perform electrocardiograms (ECG) within 15 minutes of the patient’s arrival at the hospital and commence thrombolytic therapy within 1\2 hours. The GUSTO-I trial assessed the use of tissue plasminogen activator (TPA) and streptokinase for occluded arteries around the world and found that TPA is better than streptokinase in some patients. This includes younger individuals, those who come in earlier, and people who had anterior infarcts or myocardial infarction before being treated with streptokinase. Although researchers have not defined the mechanism of action for aspirin, it seems to be as effective as thrombolytic drugs and is considered a life prescription post-MI. Furthermore, evidence suggests that early treatment with angiotensin-converting enzyme (ACE) inhibitors and β-blockers can enhance long-term prognosis in patients with decreased ventricular function. However, significant evidence does not support the use of prophylactic antiarrhythmic drugs or nitrates. Recent Treatments: 1) The Development of Regenerative Heart Medicine: Regenerative biology examines how organisms create new tissue to replace or repair damaged and lost tissues. By the next generation, human genetics, stem cell technology, and reprogramming techniques will transform cardiovascular biology as we know it today. Now we can say that regenerative medicine is moving from being a concept to a reality; practical applications are coming forth into focus. Researchers classify human cells according to their regeneration capabilities. They have long thought that striated muscle cells like cardiomyocytes contributed minimally to healing after injury and had poor regenerative abilities; these kinds of cells have often healed by scarring plastic. However, almost two decades of heart regenerative medicine research have disproved this view. Researchers in this century have discovered that tiny portions of myocyte nuclei beyond the infarct area show cell division markers indicating there might be some regenerative potential in cardiomyocytes. Nevertheless, the quantity of cardiomyocyte self-regeneration stays below one percent per year, making it unlikely to suggestively influence remedial ensuing myocardial infarction. 2) Cells in Myocardial Regeneration: Researchers should obtain the ideal cells for cardiac tissue regeneration and repair from the patient, with strong control mechanisms, localized activity, and the potential to differentiate into various cardiovascular lineages. Once implanted in the damaged myocardium, these cells are expected to promote the long-term regeneration of the tissue. Several stem cell types have been explored for their potential in myocardial repair, including hematopoietic stem cells (HSCs), embryonic stem cells (ESCs), myeloid stem cells (MSCs), induced pluripotent stem cells (IPSCs), skeletal myoblasts, and endothelial progenitor cells. 3) Stem Cell Therapies
Top 5 Shocking Causes of Dispensing Errors & Prevention
Discover top causes of dispensing errors in community pharmacies & effective prevention strategies to ensure patient safety & medication accuracy. Dispensing: Dispensing is concerned with the preparation and supply of medicine Community Pharmacies: Community pharmacy, also known as retail pharmacy, is the most popular form of pharmacy that provides the general people with drugs and health advice. Today’s community pharmacists engage in a wide range of professional duties, including patient care that optimizes pharmaceutical treatment and promotes health, wellness, and disease prevention. The dispensing procedure in community pharmacy is an important aspect of ensuring the quality use of medications, and it is one of the fundamental professional tasks of a pharmacist, along with patient counseling. Community pharmacists are increasingly involved in a wide range of patient care activities that optimize medication therapy and promote health, wellness, and disease prevention. This practice emphasizes patient-oriented services rather than just drug product delivery. Community pharmacists serve as a primary source of scientifically accurate drug information and must advocate for the safe, appropriate, and cost-effective use of medications. The dispensing process in community pharmacy is a crucial aspect of effective medication use, alongside patient counseling, forming the core professional activities of a pharmacist. The National Coordinating Council for Medication Error Reporting and Prevention (NCC MERP) defines medication error as “any preventable match that can also motive or lead to inappropriate medicine use or affected person damage whilst the medication is in the manage of the fitness care professional, patient, or consumer. Medication errors are among the most common types of medical mistakes and can occur at multiple stages of healthcare. They include errors in prescribing, transcribing, dispensing, and administration. Such incidents may be linked to various aspects of professional practice, healthcare products, and systems, including order communication, product labeling, packaging, compounding, distribution, administration, education, monitoring, and patient use. A discrepancy between the prescriber’s interpretable written order and the crammed prescription collectively with written adjustments made by means of capacity of the pharmacist pursuant to contact with the prescriber or in compliance with pharmacy coverage or the Errors that occur when distributing or promoting prescription to patient’s or patient’s agents. definition of Dispensing Errors There are so many definitions of dishing out mistakes such as: “Discrepancy between the prescriber’s written order and the stuffed prescription” or ” the Error that caught through a pharmacist observer after verification by way of the pharmacist”. The kinds of shelling out blunders suggested in the literature are: wrong drug dispensed, incorrect power dispensed, incorrect form dispensed, incorrect extent dispensed, failure to grant drug, labeling error, incorrect drug identify on label, incorrect power on label, incorrect instructions & warnings on label, incorrect volume on label, incorrect affected person identify on label and absolutely wrong label. Motives of Dispensing Errors: The literature said the following motives of dispensing errors: Comparable drug names, comparable packaging, staffing levels, bad handwriting, interruptions & distractions, design of dispensary, workforce inexperience, ambiguous directions, failure to check, lack of process, job dissatisfaction and bad communication. Some more errors includes laptop software, noise; proximity of drugs on shelves, no breaks, failure to comply with fashionable operating procedures, empty stomach, tiredness, anxiety, lack of training, lack of concentration, lighting, lone worker, complicated prescription and lack of knowledge. Therefore the purpose of this learn about was once to describe the dishing out mistakes that came about at some point of the dispensing system. Management Of Dispensing Error Risk: Two fundamental ideas summarize how the risk of dispensing blunders can be managed: In the graph and everyday operation of dispensing, an necessary technique of managing chance is the implementation of hazard controls these are traits of the pharmacy that serve to give up an error from occurring, or from main to damage if it does occur. The greater various and dependable the controls, the higher organized the pharmacy will be to manipulate danger in dispensing. In widespread terms, there are 4 kinds of controls in pharmacy: Generally, the most tremendous controls are these that get rid of blunders at supply (e.g. via disposing of a company of medicine that is especially inclined to being distributed in error). The subsequent most high quality controls are these that comprise the traits that may want to provide upward thrust to an error (e.g. by means of proscribing monitored dosage gadget meting out to specific dispensary locations). The weakest controls are commonly these that area the onus on humans to take manipulate movements themselves (e.g. setting a label subsequent to an object that is inclined to being burdened for another). This does no longer suggest that solely these controls that remove blunders at supply are worthwhile, however it does imply that relying solely on a small quantity of weaker controls will restrict the capacity to deal with the vary of mistakes that should occur. It is vital to be aware that some of the methods in which blunders would possibly show up may also now not be at once obvious. Dispensing Error: Dispensing errors are defined as any inconsistencies or deviations from the prescription order, such as dispensing the incorrect drug, dose, or dosage form, dispensing the incorrect quantity, inappropriate, incorrect, or inadequate labeling. Also confusing, or inadequate medication use instructions, and incorrect preparation, packaging, or storage of medication before dispensing are all considered as dispensing errors. Dispensing Errors In Community Pharmacies: The following are the most often reported mistakes in community pharmacies: CAUSES OF DISPENSING ERRORS: The causes of dispensing errors are discussed below: 1) Use Of Expired Products: Usually arises as a result of incorrect preparation storage, leading in degradation or the usage of expired items. 2) Wrong Preparation: This mistake is most commonly seen during compounding or other types of preparation prior to final administration. Choosing the inappropriate diluent to reconstitute is one of the examples. 3) Wrong Strength: Incorrect strength might occur at any step throughout the drug procedure. It frequently happens as a result of human mistake when comparable bottles or syringes with the wrong strength are used. 4)